Most men dismiss the first signs of prostate trouble as normal aging. A slightly weaker urine stream, waking up once or twice at night, taking a bit longer in the bathroom — these feel unremarkable. That normalization is exactly why prostate problems so often go unaddressed until they’ve progressed significantly.
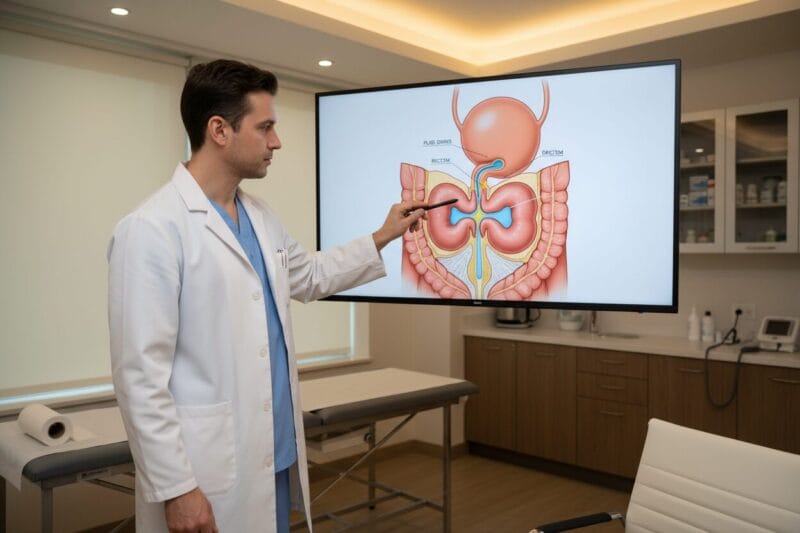
The prostate gland, a walnut-sized structure sitting just below the bladder, can begin causing noticeable changes in a man’s body years before a formal diagnosis. Recognizing those changes early, and understanding what they might mean, is one of the most important things a man can do for his long-term health.
This guide breaks down the early signs of prostate problems in men, explains what conditions those signs may indicate, and tells you clearly when it’s time to call a doctor.
The Three Prostate Conditions You Need to Know
Before diving into symptoms, it helps to understand that “prostate problems” isn’t a single diagnosis. Three distinct conditions share overlapping symptoms but have different causes, risks, and treatments.
Benign Prostatic Hyperplasia (BPH): A non-cancerous enlargement of the prostate that affects a significant portion of men over 50, with prevalence climbing sharply each decade. BPH is not cancer and doesn’t increase cancer risk, but it can seriously disrupt quality of life.
Prostatitis: Inflammation of the prostate, often caused by bacterial infection. It can be acute or chronic and, unlike BPH, can affect men of any age. Pain alongside urinary symptoms is a common feature.
Prostate cancer: The most serious of the three, and one of the most common cancers in men. Early-stage prostate cancer often produces no symptoms at all. As the Urology Care Foundation notes, when symptoms do occur, they can closely mirror those of BPH, which makes regular screening critical.
Understanding which condition a symptom cluster points toward helps you respond appropriately rather than either panicking or dismissing a genuine warning sign.
Urinary Symptoms: The Most Common Early Warning Signs
Urinary changes are the dominant early indicator across all three prostate conditions. The prostate wraps around the urethra, the tube that carries urine out of the body. When the prostate enlarges or becomes inflamed, it physically compresses the urethra, restricting flow and triggering a cascade of related symptoms.
- A weak or interrupted urine stream that requires straining to maintain
- Difficulty starting urination, even when the urge is strong
- Frequent urination, particularly every hour or two during the day
- Nocturia, meaning waking up two or more times per night to urinate
- A persistent feeling that the bladder hasn’t fully emptied after urinating
The National Institute on Aging specifically flags nocturia as a clinically significant symptom that men routinely dismiss as “just getting older.” Getting up multiple times per night isn’t a normal part of aging — it’s your body signaling that something may be compressing or irritating your urinary tract.
Dribbling after urination and sudden, urgent urges that are difficult to control are also common early indicators, particularly with BPH and prostatitis.
How Symptom Presentation Differs by Condition
The urinary symptoms above appear across BPH, prostatitis, and prostate cancer. But the pattern and accompanying signs differ in ways that can help you and your doctor narrow down what’s happening.
BPH symptoms tend to develop gradually over months or years. A weak stream and incomplete emptying are typically the most prominent complaints. There’s usually no pain, no fever, and no blood in the urine. Symptoms worsen slowly and may go unnoticed until they significantly affect daily life or sleep.
Prostatitis symptoms often come on faster and include pain that BPH doesn’t typically cause. Burning during urination, pelvic discomfort, pain in the perineum (the area between the scrotum and rectum), and sometimes lower back pain are characteristic of prostatitis. Acute bacterial prostatitis may also produce fever, chills, and flu-like symptoms requiring urgent treatment.
Prostate cancer in its early stages frequently mirrors BPH so closely that the two are indistinguishable by symptoms alone. This is why the Urology Care Foundation and MD Anderson Cancer Center’s guidance on prostate cancer warning signs both emphasize that PSA testing and clinical examination are essential rather than optional.
Pain Symptoms and What They Signal
Pain is a more specific indicator that helps distinguish between conditions and assess severity. Not all prostate problems cause pain, but when it’s present, its location and character carry real diagnostic meaning.
Burning or painful urination (dysuria) most commonly points to prostatitis, particularly bacterial prostatitis. It can also indicate a urinary tract infection or, less commonly, early prostate cancer.
Pelvic or perineal pain — a dull ache or pressure in the lower abdomen, groin, or between the legs — is strongly associated with prostatitis, including the chronic non-bacterial form, which is actually the most common type.
Bone pain in the hips, lower back, or pelvis is a different matter entirely. According to the Mayo Clinic, bone pain in these areas can indicate metastatic prostate cancer, meaning cancer that has spread beyond the prostate. Any unexplained, persistent bone pain in a man over 50 warrants urgent medical attention.
The key distinction: localized pelvic discomfort often points to prostatitis; bone pain at multiple sites suggests cancer that may have spread.
Blood in Urine or Semen
Finding blood in your urine (hematuria) or semen (hematospermia) is alarming, and it should be taken seriously. Both can be associated with prostate problems, though neither is exclusive to the prostate.
Blood in the urine may indicate prostate cancer, prostatitis, a urinary tract infection, kidney stones, or other urological conditions. The presence of blood alone doesn’t confirm a prostate problem, but it always warrants prompt medical evaluation.
Blood in semen is less commonly discussed but is a documented warning sign associated with prostate cancer and prostatitis. It’s often described as a pinkish or reddish tint to ejaculate. While it can result from minor vessel irritation in younger men, in men over 40 it should trigger a conversation with a urologist without delay.
As the NIH’s National Institute on Aging outlines in its overview of prostate problems, both blood in urine and blood in semen are listed as key warning signs that distinguish potentially serious prostate conditions from routine urinary complaints.
Sexual Dysfunction as a Prostate Indicator
Sexual health changes are among the most underreported early signs of prostate problems, partly because they’re embarrassing to discuss and partly because men often attribute them to stress or age. But the prostate plays a direct role in sexual function, and changes in that function can be meaningful signals.
Erectile dysfunction appearing alongside urinary symptoms may indicate prostate disease rather than a standalone issue. Painful ejaculation is particularly associated with prostatitis and sometimes with prostate cancer. Decreased ejaculatory volume and reduced libido can also accompany prostate conditions, especially when surrounding nerves or hormone balance is affected.
None of these symptoms alone confirms a prostate problem. But when sexual dysfunction co-occurs with urinary changes, that combination significantly raises the likelihood that the prostate is involved and should be evaluated.
Symptoms That Are Often Silent: The Case for Screening
One of the most critical facts about prostate health is that early-stage prostate cancer frequently produces no symptoms whatsoever. A man can have localized prostate cancer with a normal urine stream, no pain, and no blood in his urine. This isn’t rare — it’s the norm for early-stage disease.
This is precisely why screening matters. The two primary tools are the PSA (prostate-specific antigen) blood test and the digital rectal exam (DRE). PSA testing can detect elevated protein levels produced by prostate tissue, including cancerous tissue, before symptoms ever develop. A DRE allows a physician to physically feel the prostate for abnormalities in size, shape, or texture.
Most major health organizations recommend men discuss PSA screening with their doctor starting at age 50 for average-risk individuals. Men with a first-degree relative diagnosed with prostate cancer, or Black men who face a significantly higher risk, should have that conversation starting at age 40 to 45.
Waiting for symptoms before pursuing screening is a flawed strategy when the most treatable form of the disease often announces itself only through a blood test.
When to See a Doctor: A Practical Decision Guide
Most men miss the early signs of prostate problems specifically because they normalize symptoms that are actually clinically significant. Here’s a straightforward framework for knowing when to act.
- See a doctor within the week if you notice blood in your urine or semen, experience painful urination alongside fever or chills, or have sudden difficulty urinating.
- Schedule an appointment within the month if you’ve noticed a progressively weakening urine stream, increasing urinary frequency (especially at night), or a persistent feeling of incomplete bladder emptying lasting more than a few weeks.
- Discuss at your next routine visit if you’re over 40 and haven’t had a PSA conversation with your physician, or if you have a family history of prostate cancer.
- Seek urgent care immediately if you experience sudden inability to urinate (acute urinary retention), severe pelvic pain, or bone pain in the hips or lower back with no clear explanation.
The common thread: don’t wait for symptoms to become unbearable. Early evaluation is almost always better than delayed intervention.
Risk Factors That Should Raise Your Alertness
Certain men need to be more vigilant about recognizing early signs of prostate problems. Age is the most significant factor, with BPH and prostate cancer risk both increasing substantially after 50. But age isn’t the only variable.
Family history matters considerably. Having a father or brother with prostate cancer roughly doubles a man’s risk, and having multiple first-degree relatives with the disease raises it further.
Race is a critical and often underemphasized factor. Black men in the United States have the highest incidence and mortality rates for prostate cancer of any demographic group, due to a combination of biological differences in tumor aggressiveness and systemic barriers to early screening. If you’re a Black man, earlier and more frequent screening conversations with your doctor aren’t just recommended — they’re essential.
Diet and lifestyle also appear to influence prostate health. Diets high in red meat and processed foods, obesity, and sedentary behavior have been associated with elevated prostate cancer risk in multiple studies. Incorporating plant-based foods, maintaining a healthy weight, and staying physically active represent reasonable preventive steps alongside symptom awareness.
What Your Doctor Will Actually Look For
Understanding the clinical process removes one of the most common barriers to getting checked: many men avoid the doctor simply because they don’t know what to expect. During a prostate evaluation, your doctor will likely ask about urinary symptom frequency, severity, and duration, then order a PSA blood test and perform a digital rectal exam to assess prostate size and texture.
If PSA levels are elevated or the DRE reveals abnormalities, further testing such as an MRI or biopsy may follow. A slightly elevated PSA alone doesn’t mean cancer — BPH and prostatitis also raise PSA levels. The clinical picture is always evaluated as a whole.
Some physicians use the International Prostate Symptom Score (IPSS), a validated self-assessment questionnaire covering seven urinary symptoms on a severity scale. It’s a useful tool for quantifying how much symptoms are affecting daily life and tracking changes over time. Ask your doctor about it if you’re experiencing urinary complaints.
For men who want a broader understanding of how prostate supplements and support products fit into a prostate health routine, our complete prostate health supplement guide covers the evidence on key ingredients and what to realistically expect.