According to the American Thyroid Association, as many as 1 in 8 women will develop a thyroid disorder during her lifetime. Yet up to 60% of people living with thyroid disease have no idea anything is wrong. The symptoms are easy to dismiss: fatigue that feels like burnout, weight changes blamed on age, mood shifts written off as stress.
What makes this especially complicated for women is that thyroid dysfunction rarely works in isolation. It pulls other hormones off balance, creating a cascade of effects that touches nearly every system in the body. Understanding the signs means looking beyond the standard checklist and examining how this small gland at the base of your throat influences estrogen, progesterone, cortisol, and reproductive health.
What the Thyroid Actually Does to Your Hormones
The thyroid produces two primary hormones: thyroxine (T4) and triiodothyronine (T3). These regulate metabolism, body temperature, heart rate, digestion, and energy production at the cellular level. Every cell in your body has thyroid hormone receptors, so when output drops or surges, the effects are widespread.
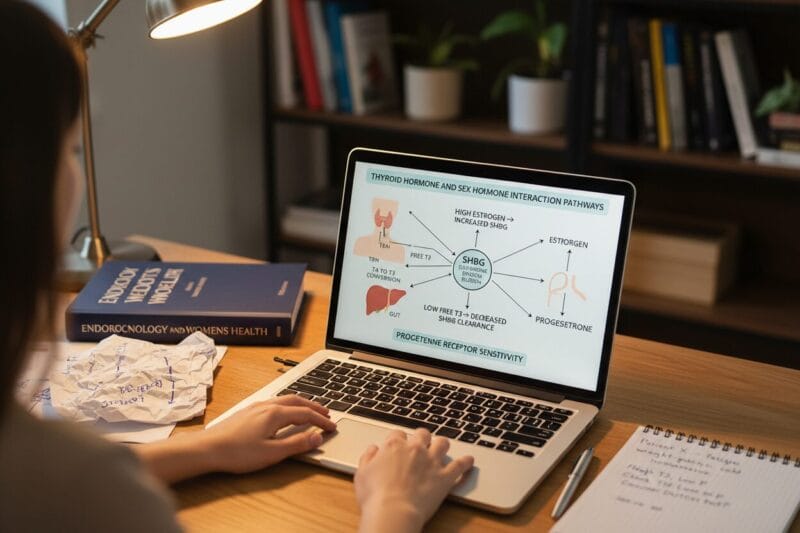
What makes this especially relevant for women is the relationship between thyroid hormones and sex hormones. Thyroid dysfunction raises levels of sex hormone-binding globulin (SHBG), a protein that binds to estrogen and testosterone and makes them less available for the body to use. When SHBG is elevated due to low thyroid function, free estrogen and testosterone drop, even when total hormone levels appear normal on a basic blood panel.
Low T3 and T4 also impair the liver’s ability to clear excess estrogen, which can contribute to estrogen dominance even when the ovaries are producing normal amounts. This estrogen-progesterone imbalance amplifies PMS symptoms, disrupts cycle regularity, and can worsen conditions like fibroids and endometriosis. The relationship runs both ways, too: high estrogen levels from pregnancy, hormone therapy, or certain health conditions increase thyroid-binding globulin, reducing free T4 availability and potentially triggering hypothyroid symptoms.
Why Women Are Disproportionately Affected
Women are 5 to 8 times more likely than men to develop thyroid disease, and the gap isn’t coincidental. Several biological factors converge to make the female thyroid more vulnerable.
The autoimmune connection is central. Hashimoto’s thyroiditis, the most common cause of hypothyroidism in women, is an autoimmune condition where the immune system attacks thyroid tissue. Women are far more susceptible to autoimmune diseases in general, partly because estrogen influences immune activity, and partly due to genetic factors on the X chromosome. Hashimoto’s often goes undiagnosed because standard TSH tests can appear normal in early stages while the immune attack is already underway.
Life transitions amplify the risk at every stage. Puberty, pregnancy, postpartum recovery, perimenopause, and postmenopause all involve hormonal shifts that stress thyroid function. Postpartum thyroiditis, for example, affects roughly 5 to 10% of women in the year after delivery, often cycling through hyperthyroid and hypothyroid phases that closely mimic postpartum depression or anxiety.
Classic Signs of an Underactive Thyroid (Hypothyroidism)
Hypothyroidism is by far the more common presentation in women. When T3 and T4 levels fall too low, metabolism slows at the cellular level because mitochondria produce less ATP, the body’s primary energy currency. This is why the fatigue of hypothyroidism feels different from ordinary tiredness; it’s a deep, cellular exhaustion that sleep doesn’t fully resolve.
The most frequently reported signs include:
- Persistent fatigue and low energy that worsens throughout the day
- Unexplained weight gain or difficulty losing weight despite normal diet and exercise
- Feeling cold when others are comfortable, particularly in the hands and feet
- Brain fog, poor concentration, and memory lapses
- Dry skin, brittle nails, and coarse or thinning hair
Beyond these hallmarks, hypothyroidism produces several hormone-specific symptoms women often attribute to other causes. Heavy or irregular periods, difficulty conceiving, low libido, vaginal dryness, and worsening PMS are all downstream effects of disrupted thyroid-estrogen-progesterone balance. Depression and emotional flatness are also common; reduced T3 affects serotonin receptor sensitivity in the brain, altering mood regulation independently of life circumstances.
Signs of an Overactive Thyroid and Its Hormonal Effects
Where hypothyroidism slows everything down, hyperthyroidism accelerates it. The most common cause in women is Graves’ disease, another autoimmune condition. As the Rush University Medical Center clinical team notes, “anxiety, restlessness, irritability and insomnia can signal hyperthyroidism, while depression, fatigue, low energy and forgetfulness may point to hypothyroidism.”
Hyperthyroidism increases the rate at which the body metabolizes estrogen, which can lower estrogen levels and disrupt the luteal phase of the menstrual cycle. This often presents as lighter periods, shorter cycles, or missed periods entirely. Bone density also takes a hit because excess thyroid hormone accelerates bone turnover, increasing fracture risk over time.
Key signs that thyroid activity may be too high include:
Rapid or irregular heartbeat: Often described as palpitations or a fluttering sensation in the chest
Unexplained weight loss: Despite a normal or increased appetite, the body burns through energy too quickly
Heat intolerance and excessive sweating: The body runs hot even in cool environments
Anxiety that feels physical: Restlessness, trembling hands, and a sense of internal agitation rather than situational worry
Eye changes or neck swelling: Particularly common when Graves’ disease is the underlying cause
How Thyroid Dysfunction Affects Your Cycle and Fertility
The menstrual cycle is one of the most sensitive indicators of thyroid health in women of reproductive age. Both hypothyroidism and hyperthyroidism disrupt the hypothalamic-pituitary-ovarian (HPO) axis, the hormonal feedback loop that governs ovulation and cycle regularity.
In hypothyroidism, elevated TSH stimulates the pituitary to release more prolactin, a hormone normally associated with breastfeeding. Elevated prolactin suppresses ovulation, which can cause irregular or absent periods and make conception difficult. This is why thyroid function testing is a standard part of fertility workups.
The thyroid-PCOS connection is also worth understanding. Hypothyroidism can worsen insulin resistance, increase androgen levels, and produce a hormonal profile that mimics polycystic ovary syndrome. Some women are treated for PCOS for years before an underlying thyroid issue is identified. Thyroid problems in women and their hormonal symptoms are often intertwined in ways that require comprehensive testing rather than treating each condition in isolation.
Thyroid Symptoms Mistaken for Perimenopause
One of the most underrecognized clinical problems is the overlap between thyroid dysfunction and perimenopause. Both conditions share a striking number of symptoms: fatigue, weight changes, mood swings, brain fog, irregular periods, sleep disturbances, and temperature sensitivity. Women in their 40s are frequently told their symptoms are “just perimenopause” when thyroid dysfunction is the primary or contributing cause.
The cortisol-thyroid connection adds another layer of complexity. Chronic stress elevates cortisol, which directly suppresses the conversion of T4 to the active T3 form. It also increases Reverse T3 (rT3), an inactive thyroid hormone that competes with T3 at receptor sites and blocks its effects. A woman can have technically “normal” TSH and T4 levels while still experiencing significant hypothyroid symptoms if her T3 conversion is impaired by chronic stress or adrenal dysfunction.
This is why symptoms that persist despite normal TSH results deserve further investigation, not dismissal. The signs of thyroid trouble explained by Rush University Medical Center reinforce that mood and energy changes are often the first signals women notice, frequently years before a formal diagnosis.
Thyroid Nodules and When to Take Symptoms Seriously
Most thyroid dysfunction is benign and manageable, but some symptoms warrant prompt medical evaluation. Thyroid nodules are extremely common in women, and the vast majority are non-cancerous. However, certain signs suggest the need for imaging and biopsy.
- A visible lump or swelling at the base of the throat
- Difficulty swallowing or a persistent sensation of pressure in the neck
- Hoarseness or voice changes without an obvious cause
- Swollen lymph nodes in the neck that don’t resolve
Thyroid cancer is relatively rare but is diagnosed more frequently in women than men. Most thyroid cancers are highly treatable when caught early, so any new neck lump or persistent swallowing difficulty should be evaluated by a physician, regardless of whether other thyroid symptoms are present.
What Tests to Ask For and What the Results Mean
Standard thyroid screening typically includes only TSH, but a single TSH number gives an incomplete picture of thyroid hormone function, particularly for women whose symptoms involve the broader hormonal system. A comprehensive thyroid panel should include:
TSH (Thyroid-Stimulating Hormone): The pituitary signal that tells the thyroid to produce hormones. Elevated TSH suggests underperformance; suppressed TSH suggests overactivity.
Free T4 (FT4): The storage form of thyroid hormone. Low FT4 with high TSH confirms hypothyroidism.
Free T3 (FT3): The active form cells actually use. Some women convert T4 to T3 poorly, meaning FT3 can be low even when FT4 appears adequate.
Reverse T3 (rT3): An inactive form that blocks T3 receptors. Elevated rT3 is common in chronic stress and can explain persistent symptoms despite otherwise normal labs.
TPO Antibodies (Anti-TPO): Elevated antibodies confirm Hashimoto’s thyroiditis, the autoimmune form of hypothyroidism, which requires different management than non-autoimmune hypothyroidism.
Advocating for a complete panel rather than TSH alone is one of the most important steps a woman can take when symptoms point to thyroid involvement. If a physician is reluctant to run the full panel, requesting a referral to an endocrinologist is a reasonable next step. If you’re exploring at-home testing options alongside traditional care, reviewing a comprehensive thyroid health test guide can help you understand what each marker means before your appointment.
Lifestyle Factors That Disrupt Thyroid Hormone Production
Several modifiable factors directly affect how well the thyroid produces and converts hormones. Iodine deficiency remains a global cause of hypothyroidism, though it’s less common in countries with iodized salt. More relevant to most women are the following influences.
Chronic sleep deprivation suppresses TSH secretion and reduces T3 levels. Selenium deficiency impairs the conversion of T4 to active T3; selenium is found in Brazil nuts, eggs, and seafood. Excess soy consumption and large quantities of raw cruciferous vegetables can interfere with iodine uptake in iodine-deficient individuals, though this is rarely a concern for women with adequate iodine intake.
Environmental endocrine disruptors, including BPA in plastics, PFAS chemicals in non-stick cookware, and certain pesticides, have been shown to interfere with thyroid hormone signaling at the receptor level. Fluoride and chlorine in drinking water may also affect iodine absorption over time. These aren’t reasons for alarm, but they’re worth factoring into an overall approach to thyroid health, particularly for women already managing borderline thyroid function.
What to Do If You Recognize These Signs
Recognizing the signs is the first step; knowing what to do next is what matters. The Office on Women’s Health notes that “depending on how much or how little hormone your thyroid makes, you may often feel restless or tired, or you may lose or gain weight,” which captures how variable and easy to overlook these symptoms can be.
If several of the signs in this article resonate with your experience, here’s a practical sequence to follow:
- Document your symptoms in writing, noting when they started, their severity, and any patterns tied to your menstrual cycle or stress levels.
- Request a comprehensive thyroid panel from your primary care physician or OB-GYN, specifically asking for TSH, Free T3, Free T4, and TPO antibodies.
- Ask about Reverse T3 testing if your symptoms persist despite normal standard results.
- Request that results be shared numerically, not just as “normal” or “abnormal,” so you can track changes over time.
- If your physician dismisses symptoms without testing, seek a second opinion from an endocrinologist or functional medicine practitioner with thyroid experience.
Treatment for hypothyroidism typically involves synthetic T4 (levothyroxine), though some women respond better to combination T3/T4 therapy or desiccated thyroid extract. Hyperthyroidism treatment options include antithyroid medications, radioactive iodine, or surgery, depending on the cause and severity.